 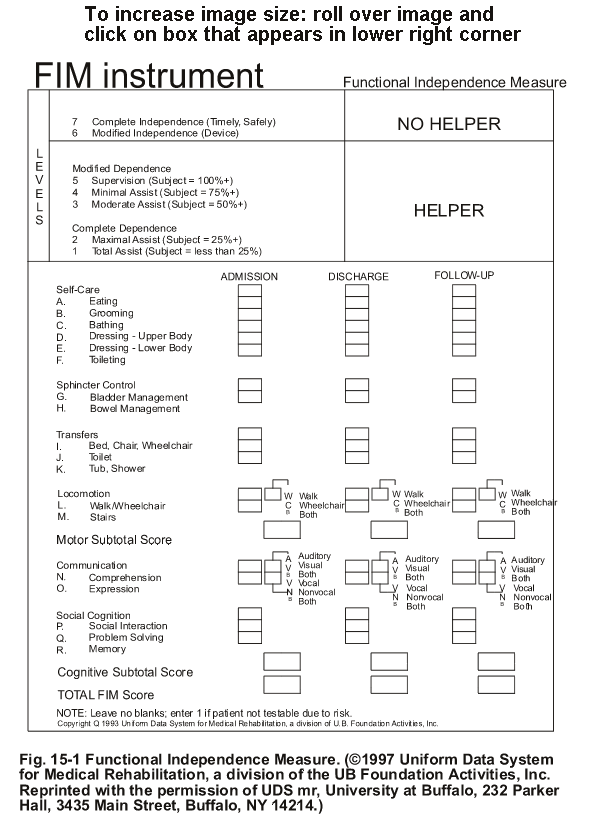 
Īlthough functional status has been identified as a strong predictor of mortality for very elderly patients in ICUs, standard hospitalization settings, and situations involving bacteremia or pneumonia, data are very limited regarding IMCUs. An effective triage process for elderly patients before ICU or IMCU admission seems necessary and should ideally assess not only comorbidities but also functionality, which is usually difficult to determine, especially during acute organ failure. Tasks evaluated using FIM include sphincter control, transfers, locomotion, communication, social cognition, and the following six self-care activities: grooming, bathing, feeding, upper-body dressing, lower-body dressing, and toileting.Ī recent study showed that the systematic admission of critically ill elderly patients to ICUs did not reduce six-month mortality in comparison with usual practice. Total scores range from 18 (lowest) to 126 (highest level of function). FIM scores 18 items of physical, psychological, and social function from 1 to 7, assessing the patient’s level of disability and changes in status in response to rehabilitation or medical intervention. The Functional Independence Measure (FIM) provides another functional score, routinely used with geriatric patients to assess their functional status during hospitalization It is widely used in our hospital for its reliability and reproducibility. Indeed, a frailty assessment before admission to an ICU or IMCU may provide more accurate prognostic information than age and comorbidities alone. reported that Clinical Frailty Scale scores were inversely associated with the short-term survival of very elderly patients (≥ 80 years) admitted to an ICU. Frailty seems a promising predictor of mortality. The number or severity of a patient’s comorbidities is also often used by clinicians to aid triage decisions on admission to an ICU or IMCU. They help clinicians decide whether to admit a patient to an ICU or IMCU, even though their accuracy for very elderly patients is uncertain. ĭisease severity scores are well-known tools for evaluating risk of death in the short term. Better predictors of short and long-term mortality are needed to improve triage decisions. Indeed, this population’s health status is often difficult to assess because of multiple morbidities and frailty. However, several studies have suggested that age alone is not a strong predictor of mortality. Age has generally been thought to have a strong association with intensive and intermediate care outcomes, with older patients having a poorer prognosis than younger ones. This opens up perspectives on the potential value of FIM for establishing a finer prognosis and better triage of critically ill older patients.Īs the global population ages, growing numbers of elderly and very elderly patients are being admitted to intensive care units (ICUs) or intermediate care units (IMCUs). In the present study, higher functional status, assessed using the FIM tool before admission to an IMCU, was significantly and independently associated with lower one-year mortality. Multivariate survival analysis showed a significant difference between groups, with a hazard ratio of 0.29 (95% CI: 0.13–0.65) for patients with high FIM scores. Logistic regression calculations found an association between pre-admission FIM score and one-year mortality ( p < 0.0001), including variables usually associated with mortality (e.g., age, sex, comorbidities, mini-mental health state score, renal function). Dichotomized low (≤ 63) and high FIM (> 63) scores were associated with one-year mortalities of 68 and 44%, respectively. ResultsĪ total of 345 patients were included (56% female, mean age 85 +/− 6.5 years). The study’s primary outcome metrics were one-year mortality’s associations with a pre-admission FIM score and other relevant prospectively recorded prognostic variables. MethodsĪ monocentric, retrospective, observational study of all patients aged ≥75 years old admitted to Geneva University Hospitals’ geriatric IMCU between and. 
This study aimed to determine whether functional status, assessed using the Functional Independence Measure (FIM), could be an independent predictor of mortality in a geriatric population admitted to an intermediate care unit (IMCU). Chronic health status and functional status before admission could be better predictors. Age alone is not a robust predictor of mortality in critically ill elderly patients. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
